Why High-Value Medical Consumables Face Tougher Price Pressure
Why do high-value medical consumables face stronger price pressure while clinical expectations keep increasing? The answer sits at the intersection of policy, hospital economics, and technical competition.
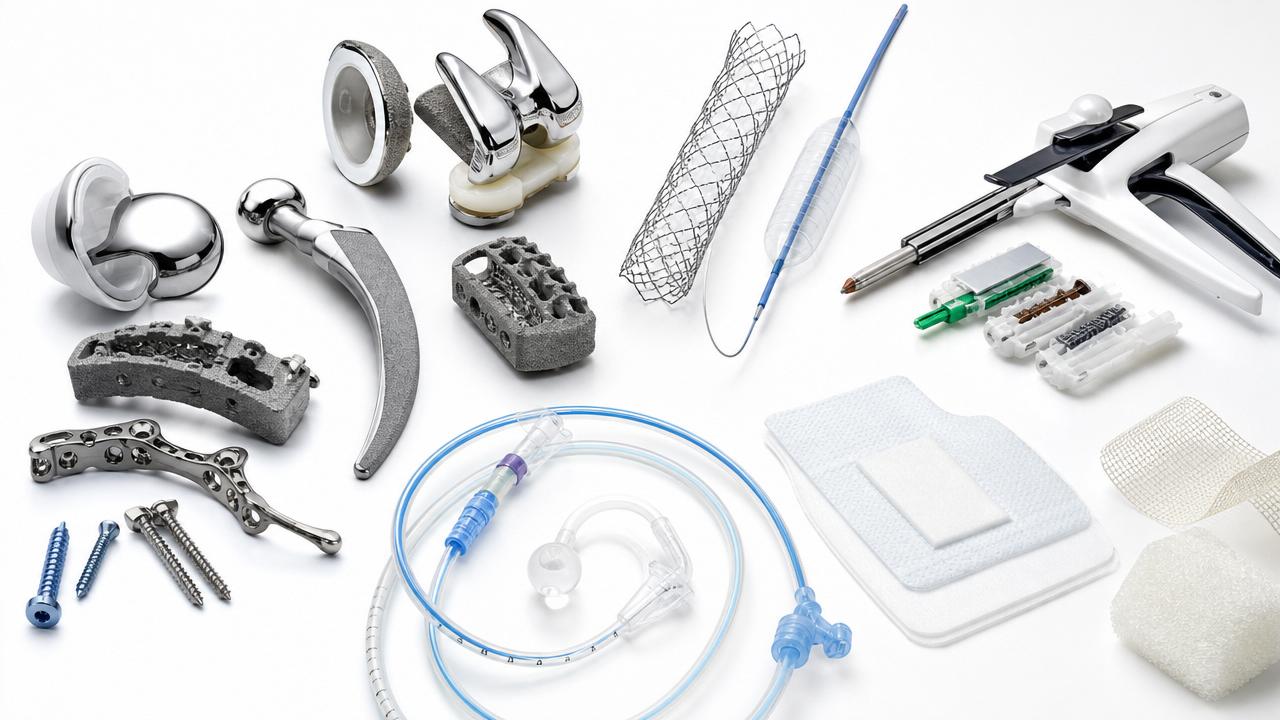
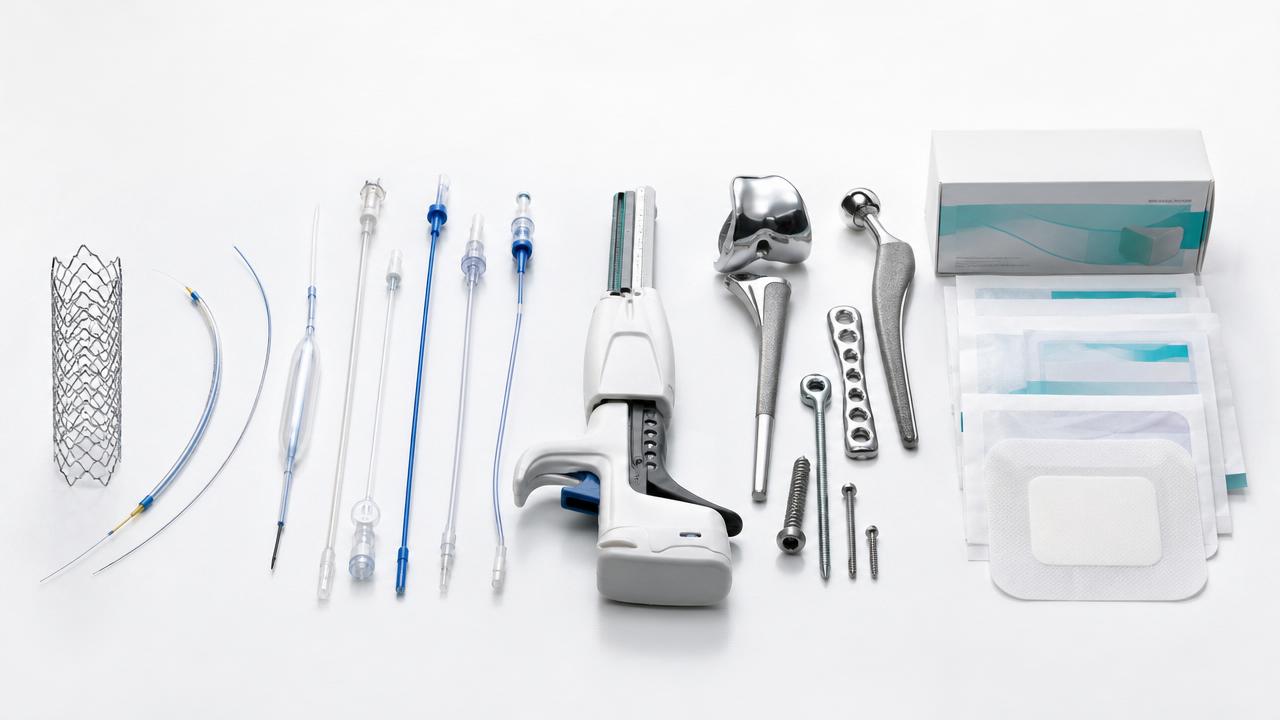
Across implants, interventional devices, staplers, catheters, and advanced wound care, buyers now compare not only performance, but also reimbursement fit, evidence quality, and supply resilience.
This shift is changing how the market values innovation. In many cases, premium pricing survives only when clinical differentiation is measurable, repeatable, and relevant to total treatment cost.
Price pressure is no longer cyclical for high-value medical consumables
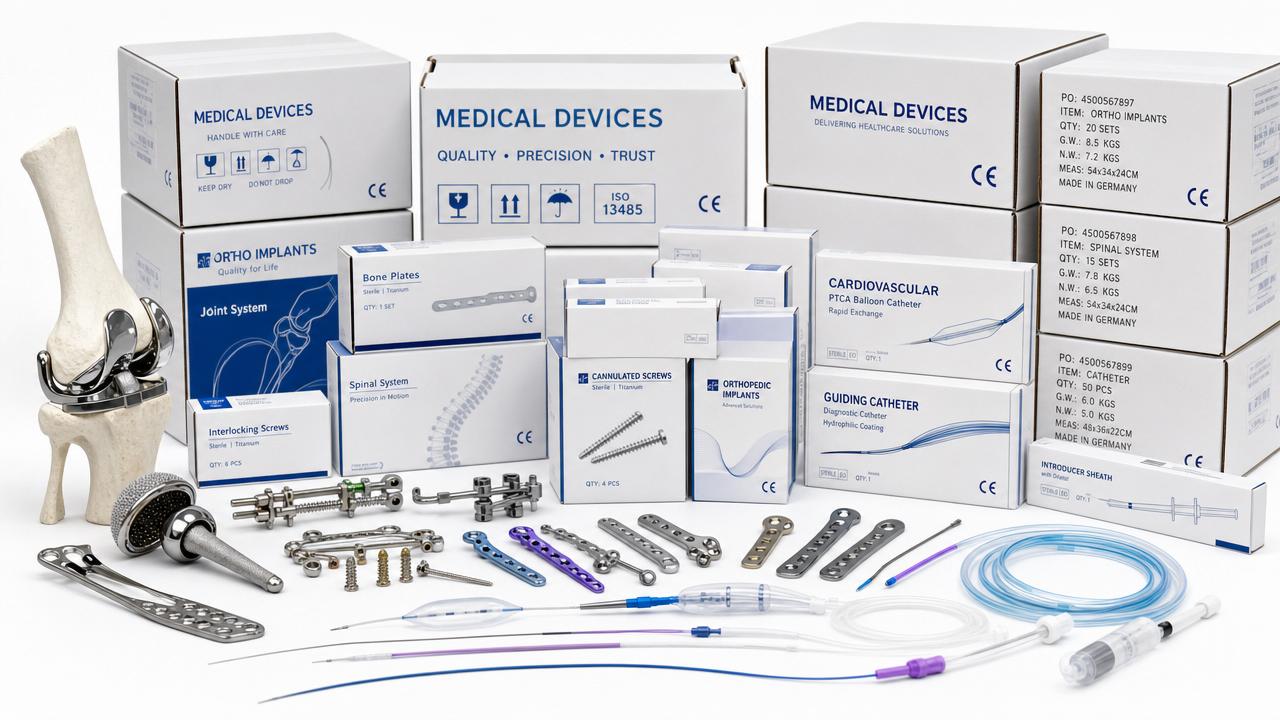
The current squeeze on high-value medical consumables is structural, not temporary. Volume-based procurement, centralized tenders, and hospital budget controls have reset pricing expectations in many regions.
At the same time, regulatory standards are becoming stricter. Class III devices need stronger clinical data, tighter traceability, and more robust quality documentation across the product lifecycle.
This creates a difficult paradox. Development, validation, and compliance costs rise, while market access increasingly rewards lower bid prices and wider supply commitments.
For categories such as orthopedic implants, DES, TAVR systems, MIS staplers, and specialty catheters, the pricing debate now extends beyond unit cost into evidence, outcomes, and operational reliability.
Several market signals explain why pricing power is weakening
The decline in pricing power for high-value medical consumables is driven by multiple forces at once. None acts alone, and together they reshape the competitive floor.
In practical terms, price is falling fastest where products look clinically interchangeable. Where differentiation is unclear, high-value medical consumables are treated more like managed cost items than strategic technologies.
Mature segments feel the earliest shock
Coronary stents, trauma fixation, standard joint systems, and widely adopted stapling platforms often experience the steepest pressure first. Clinical familiarity reduces tolerance for unexplained premium gaps.
Novel segments are not immune
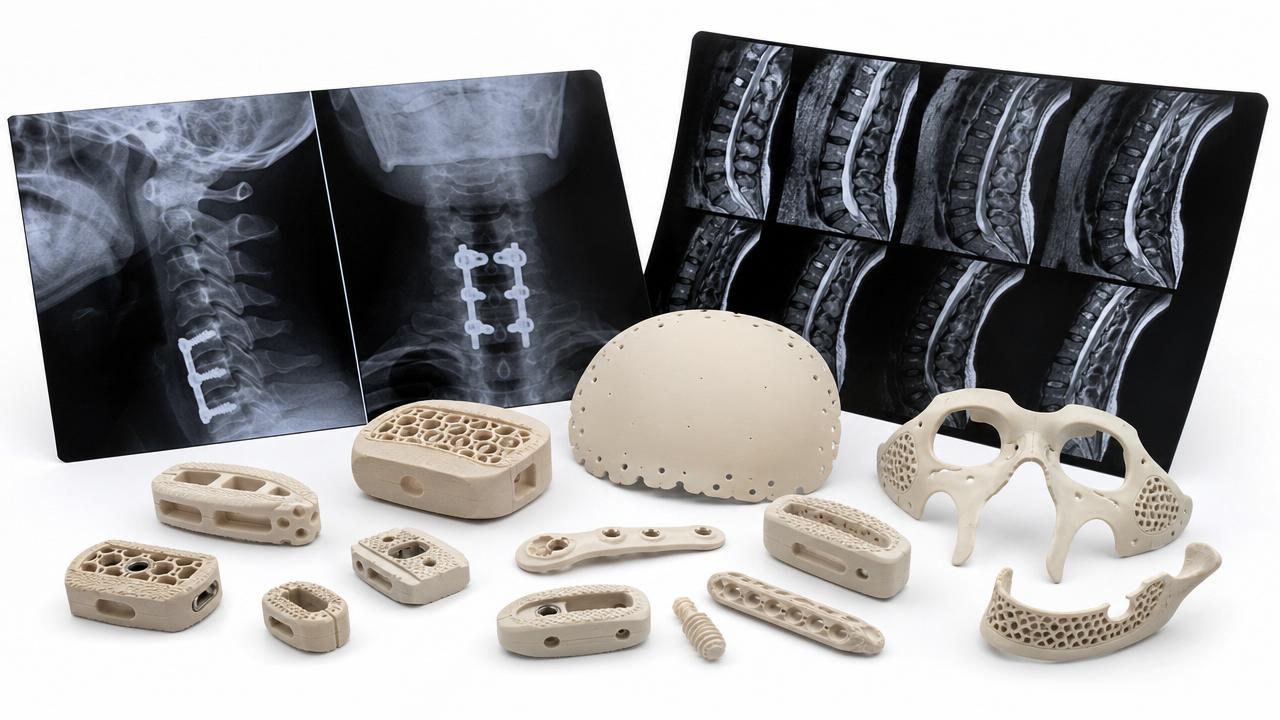
Even advanced tissue regeneration materials or complex cardiovascular devices face pricing scrutiny. Innovation alone is no longer enough if evidence does not show downstream economic value.
The real issue is how value is being redefined
The market has not stopped valuing innovation. Instead, it now demands proof that innovation reduces revision risk, shortens procedure time, lowers complications, or improves recovery quality.
For high-value medical consumables, value is shifting from technical claims to clinical and economic evidence. A coating, alloy, porous structure, or polymer blend must show practical treatment impact.
- Biocompatibility must translate into lower adverse event risk.
- Precision machining must support procedural consistency.
- Design upgrades must improve handling or long-term outcomes.
- Clinical studies must match target populations and real use settings.
- Post-market data must reinforce early performance claims.
This matters strongly in IMCS-covered categories. Orthopedic implants, cardiovascular consumables, and advanced dressings each compete under different pathways, but all now face evidence-based pricing discipline.
Different business links feel the pressure in different ways
Price pressure on high-value medical consumables does not affect every part of the chain equally. Some functions absorb direct financial stress, while others face strategic repositioning pressure.
R&D and regulatory functions
Teams must justify expensive development paths earlier. ISO 10993 validation, CER preparation, usability testing, and post-market follow-up require tighter target-product definitions from the start.
Production and supply planning
Factories face a difficult balance between lower average selling prices and the need for stable quality. Scale, scrap control, automation, and validated process repeatability become central margin levers.
Commercial and market access teams
Commercial success now depends less on brand prestige alone. Strong tender strategy, local evidence adaptation, and service support often decide whether premium products remain viable.
Clinical users and health systems
Lower prices can improve access, but excessive compression carries risks. If supply becomes unstable or training support weakens, treatment consistency may suffer despite short-term savings.
What deserves closer attention beyond unit price
When evaluating high-value medical consumables, focusing only on bid price may hide larger costs. A better approach is to review performance through a total-value lens.
- Clinical evidence depth, not just regulatory clearance.
- Complication, revision, and readmission implications.
- Procedure efficiency and operating room time impact.
- Surgeon learning curve and technical support requirements.
- Supply continuity across tender cycles and regional demand swings.
- Raw material and component traceability.
- Post-market surveillance responsiveness.
- Compatibility with reimbursement and coding structures.
This is especially relevant for implantables and interventional systems. A device that appears cheaper may create higher downstream costs if failure risk, handling difficulty, or inventory inconsistency rises.
A practical framework helps judge future pricing resilience
Not all high-value medical consumables will lose pricing power equally. Resilience usually depends on how clearly a product separates itself from standard alternatives.
The next market winners will combine compliance, proof, and cost discipline
The future of high-value medical consumables will not be decided by low price alone. Nor will it be secured by innovation claims without evidence and operational execution.
The stronger position belongs to products that unite biocompatibility, precision manufacturing, regulatory readiness, and health-economic logic. That combination is harder to replace in a tender-driven environment.
In sectors tracked by IMCS, this means watching both technology evolution and policy mechanics. A premium product remains defensible only when its technical edge survives financial scrutiny.
A useful next step is to map each category by three factors: substitution risk, evidence strength, and procurement sensitivity. That view reveals where price pressure is temporary and where it is permanent.
For any review of high-value medical consumables, start with one question: does this product lower total treatment risk in a way that can be proven? If the answer is clear, pricing discussions become more rational.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.
News Recommendations