ISO 10993 Testing Delays Often Start With Sample Prep
ISO 10993 testing delays are increasingly traced to earlier preparation steps
Many ISO 10993 testing delays do not begin in the lab. They begin during sample preparation, before any extraction, incubation, or biological endpoint is measured.
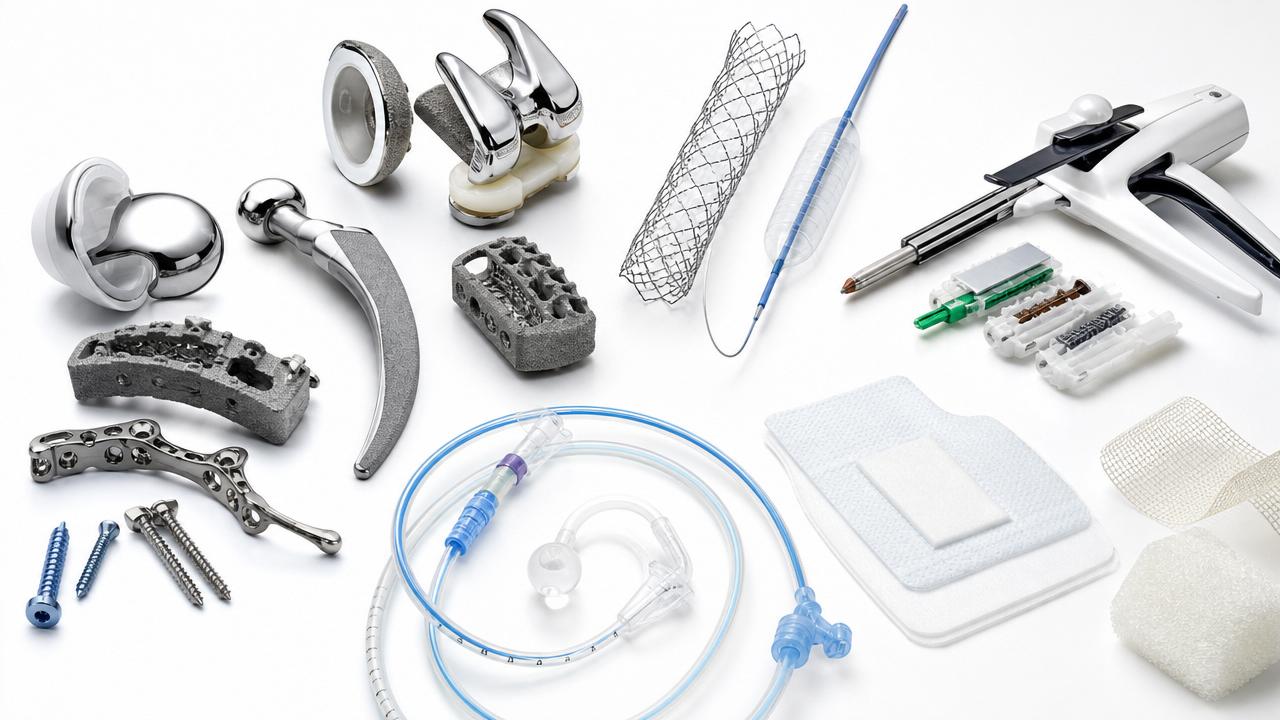
Across implants, catheters, staplers, and wound materials, weak prep control often causes failed timelines, retests, and incomplete biological risk evaluations.
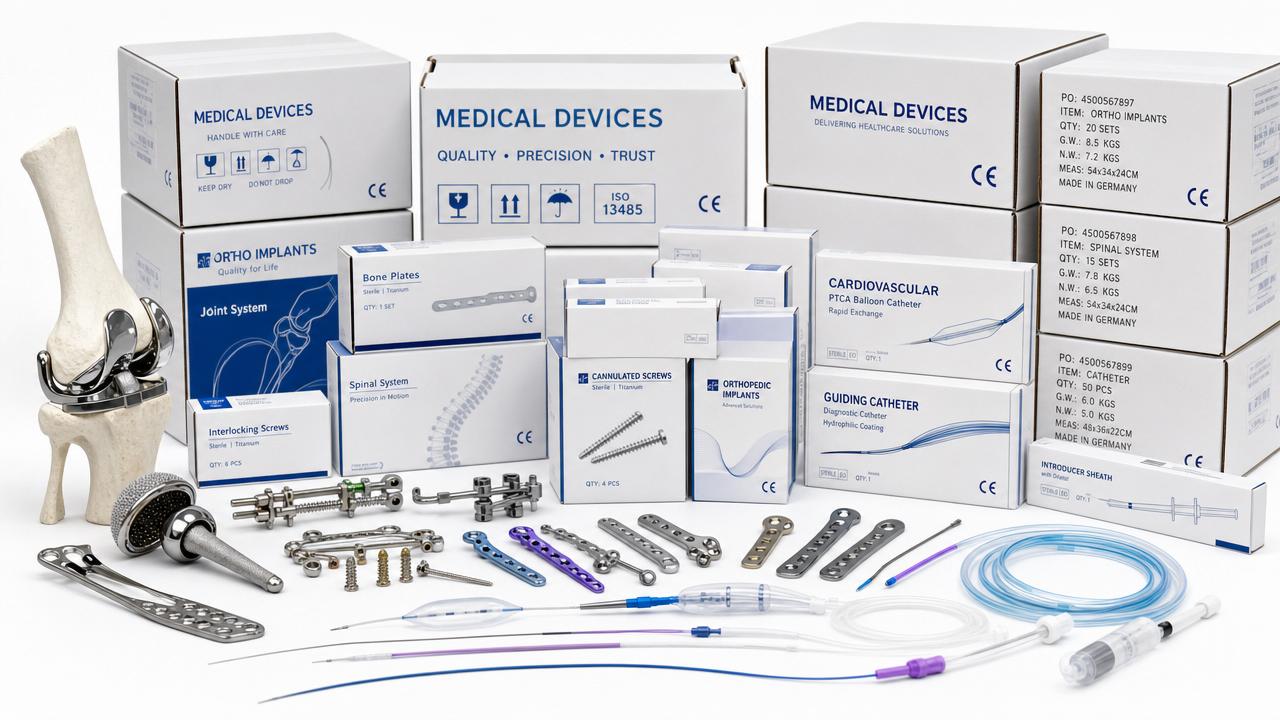
That shift matters because ISO 10993 testing is now reviewed more closely under global Class III device expectations, design changes, and stricter technical documentation practices.
For IMCS, this pattern reflects a broader industry reality. Biocompatibility success depends not only on chemistry and toxicology, but also on disciplined material handling.
A clear trend signal: preparation quality now shapes biological safety timelines
In the past, teams often treated sample preparation as a routine handoff. Today, it has become a leading predictor of ISO 10993 testing efficiency and data acceptability.
Regulators and test laboratories increasingly expect traceable preparation logic. They want to see why a sample format, extraction ratio, packaging state, and sterilization condition were selected.
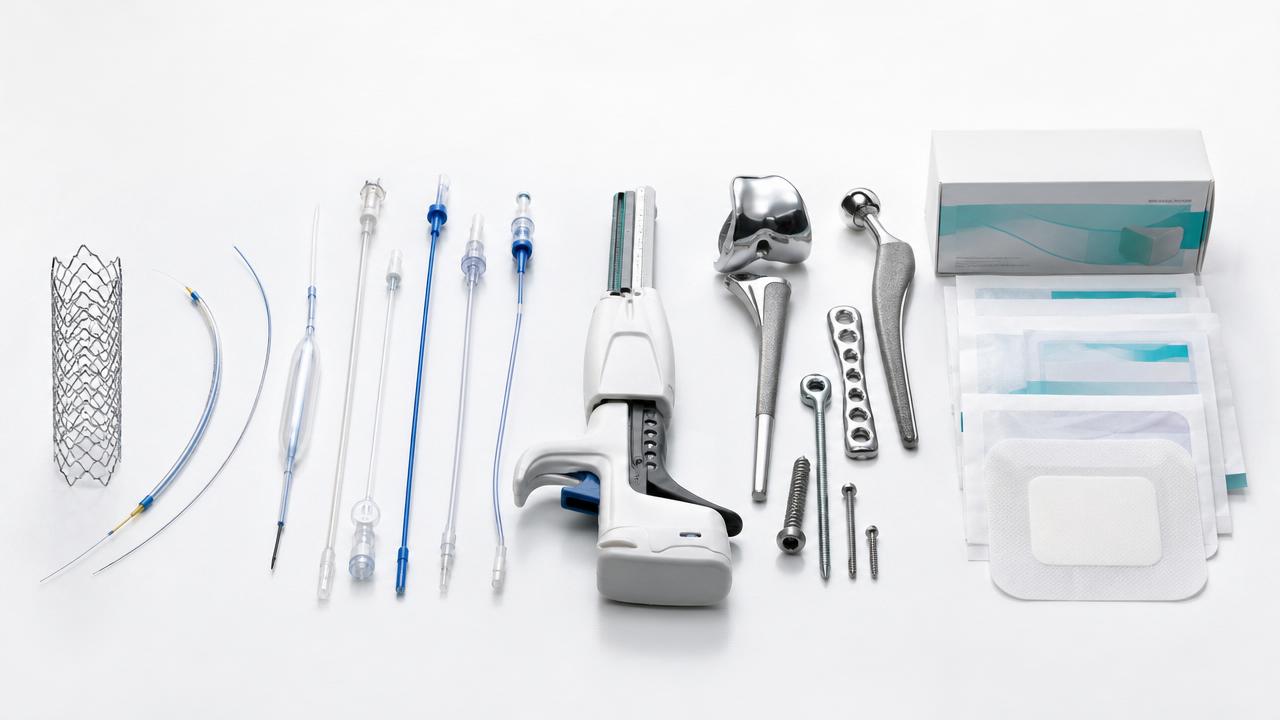
This is especially important for multi-material devices. Orthopedic implants, DES systems, polymer catheters, staplers, and advanced dressings rarely behave like simple single-substance articles.
As devices become smaller, coated, porous, drug-bearing, and combination-oriented, ISO 10993 testing becomes more sensitive to early preparation errors.
Why this signal is becoming stronger
- More complex materials increase uncertainty in extraction behavior.
- Global submissions demand stronger rationale for test article representativeness.
- Change control pressures require updated ISO 10993 testing after process or supplier shifts.
- Laboratories reject poorly documented samples more quickly than before.
- Time-to-market targets leave little buffer for repeat preparation cycles.
The most common causes behind sample prep failure in ISO 10993 testing
The drivers of delay are rarely dramatic. They are usually small, procedural mistakes that accumulate and later compromise the validity of ISO 10993 testing.
Subtle errors that often go unnoticed
A wiped implant may no longer reflect commercial cleanliness. A trimmed catheter may expose fresh polymer edges never seen in clinical use.
A dressing folded differently from final packaging may alter extractables. These small changes can distort ISO 10993 testing without obvious warning signs.
Different device categories feel the impact in different ways
The consequences of bad preparation are not identical across the medical consumables landscape. Each device family carries its own sensitivity points.
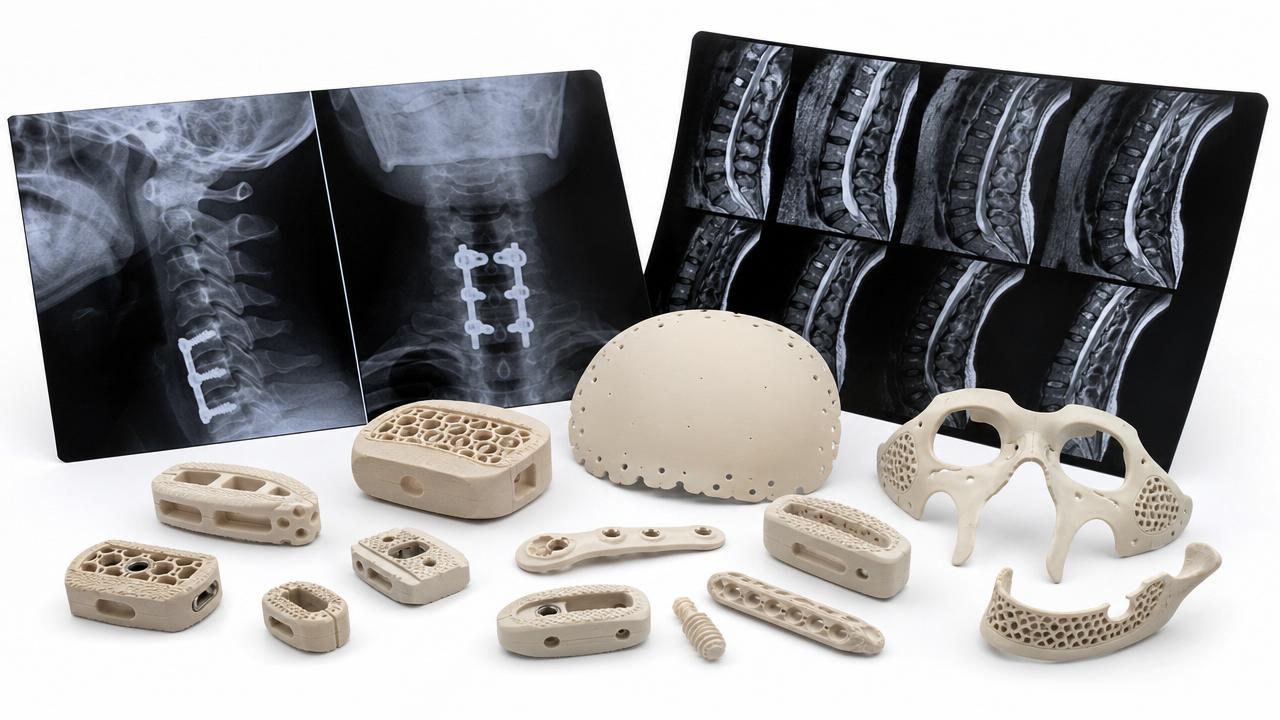
Orthopedic implants and porous structures
Porous titanium, coated fixation layers, and PEEK combinations complicate extraction logic. Surface-rich geometries may trap residues or behave differently after sterilization.
Cardiovascular interventional devices
DES systems, balloons, and valve delivery components depend heavily on coating integrity. Mishandling during sample prep may remove, crack, or contaminate critical layers.
Minimally invasive staplers and metal-polymer assemblies
These products often include lubricants, adhesives, and dissimilar materials. ISO 10993 testing may be delayed when the chosen sample fails to represent assembled-use conditions.
Polymer catheters and coated lumens
Hydrophilic and antithrombotic coatings are vulnerable during cutting and handling. Even storage conditions before dispatch can influence ISO 10993 testing outcomes.
Advanced wound care materials
Foams, alginates, silicones, and silver-based systems absorb liquids differently. Extraction preparation must consider swelling, release profiles, and contact-state realism.
The business impact goes beyond the laboratory schedule
Poor preparation affects more than one test report. It can disrupt regulatory sequencing, launch plans, internal validation windows, and technical file credibility.
When ISO 10993 testing must be repeated, associated chemistry work, toxicological assessment, and biological evaluation updates may also be delayed.
That is especially costly when design verification, packaging validation, sterilization release, and submission milestones are already tightly linked.
- Retests consume reserve samples and extend lead times.
- Documentation revisions create cross-functional rework.
- Regulatory questions may expand beyond the original endpoint.
- Supplier or process changes become harder to justify retrospectively.
What deserves closer attention before ISO 10993 testing begins
Strong programs reduce delay risk by making sample preparation a controlled technical activity, not a shipping task.
Core checkpoints worth formalizing
- Define the exact market-state sample to be tested.
- Document whether samples are cleaned, uncleaned, or process residual-bearing.
- Control cutting methods to avoid unrealistic new surfaces.
- Confirm packaging and sterilization status before dispatch.
- Align extraction rationale with contact type, duration, and material profile.
- Keep traceable labels tied to lot, revision, and manufacturing route.
- Review changes in suppliers, coatings, additives, or post-processing steps.
A practical response path can reduce ISO 10993 testing setbacks
The best response is not simply faster testing. It is earlier alignment between development, quality, toxicology, and laboratory execution.
The next competitive advantage may be preparation discipline, not just test capacity
In high-value medical consumables, biocompatibility timelines are increasingly won or lost before the lab starts. That is the deeper market signal behind rising ISO 10993 testing delays.
Preparation discipline supports stronger evidence, fewer surprises, and smoother biological evaluation across implants, interventional devices, staplers, catheters, and wound care systems.
A focused review of sample state, extraction rationale, and traceability can often prevent weeks of avoidable delay in ISO 10993 testing.
For organizations navigating complex regulations and aggressive launch windows, the next practical step is simple: audit sample preparation before scheduling the next test series.
That small shift can protect data quality, regulatory confidence, and the broader business case behind every biocompatibility program.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.
News Recommendations