Medical Device Clinical Evaluation Gaps Found Too Late
Many compliance teams discover critical medical device clinical evaluation gaps only when submission timelines are already at risk. For quality and safety managers, late findings can trigger costly rework, weak clinical justification, and regulatory delays. This article explores why these gaps are missed, where they typically emerge, and how earlier evidence planning can strengthen Class III device readiness.
Why are medical device clinical evaluation gaps often found too late?
In high-risk medical consumables, the clinical evaluation rarely fails because one document is missing. It fails because evidence, risk management, biological safety, post-market logic, and intended use were not aligned early enough.
For quality and safety managers, the issue is practical. Teams may pass design reviews, supplier audits, bench verification, and biocompatibility planning, yet still face major questions when building the medical device clinical evaluation narrative.
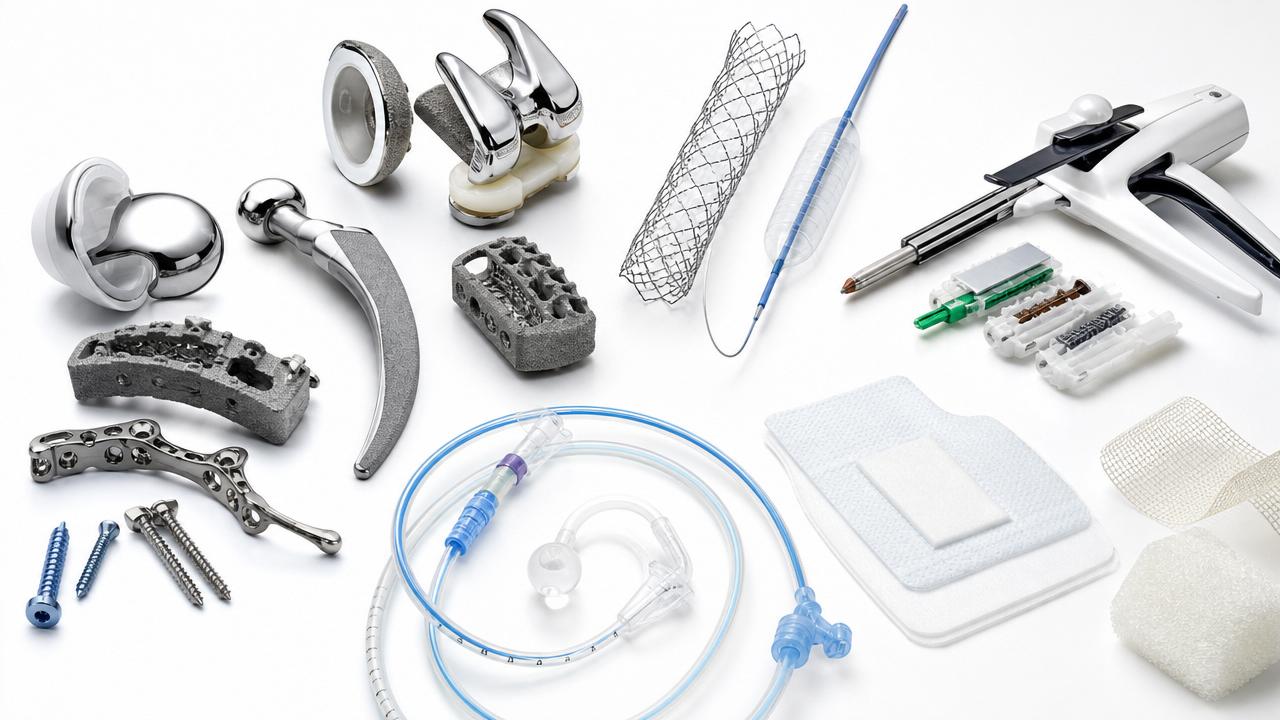
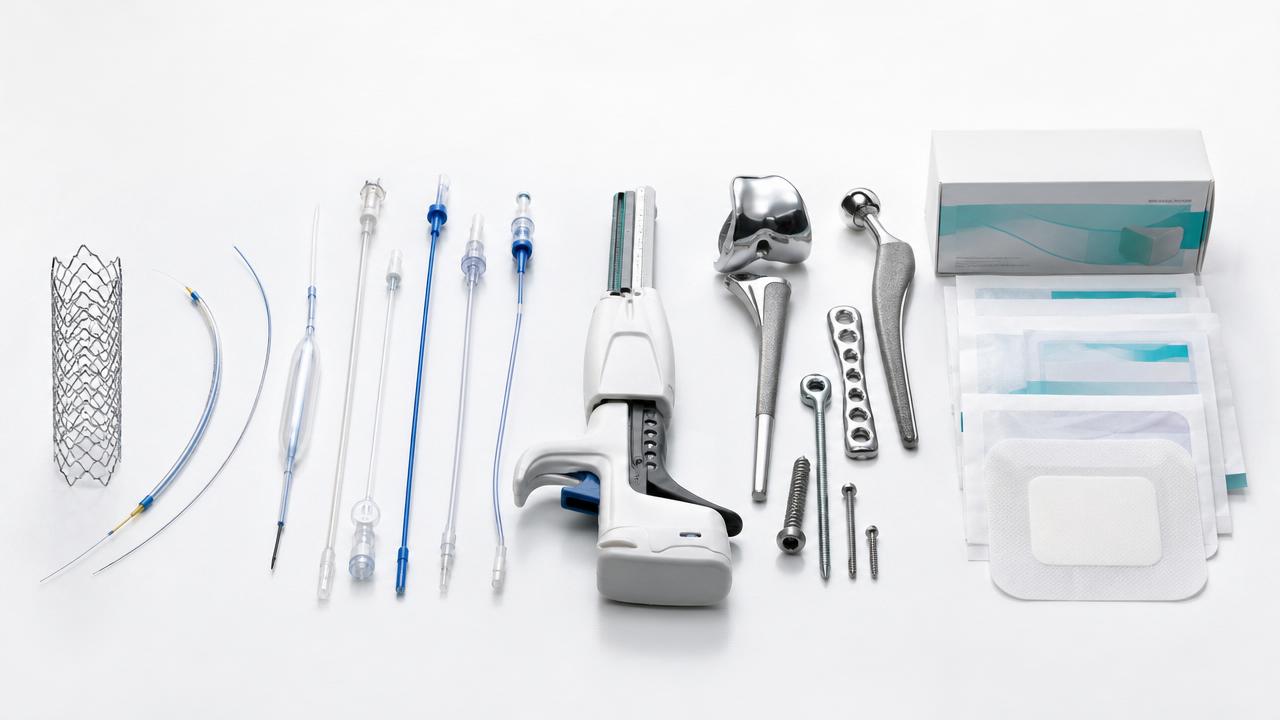
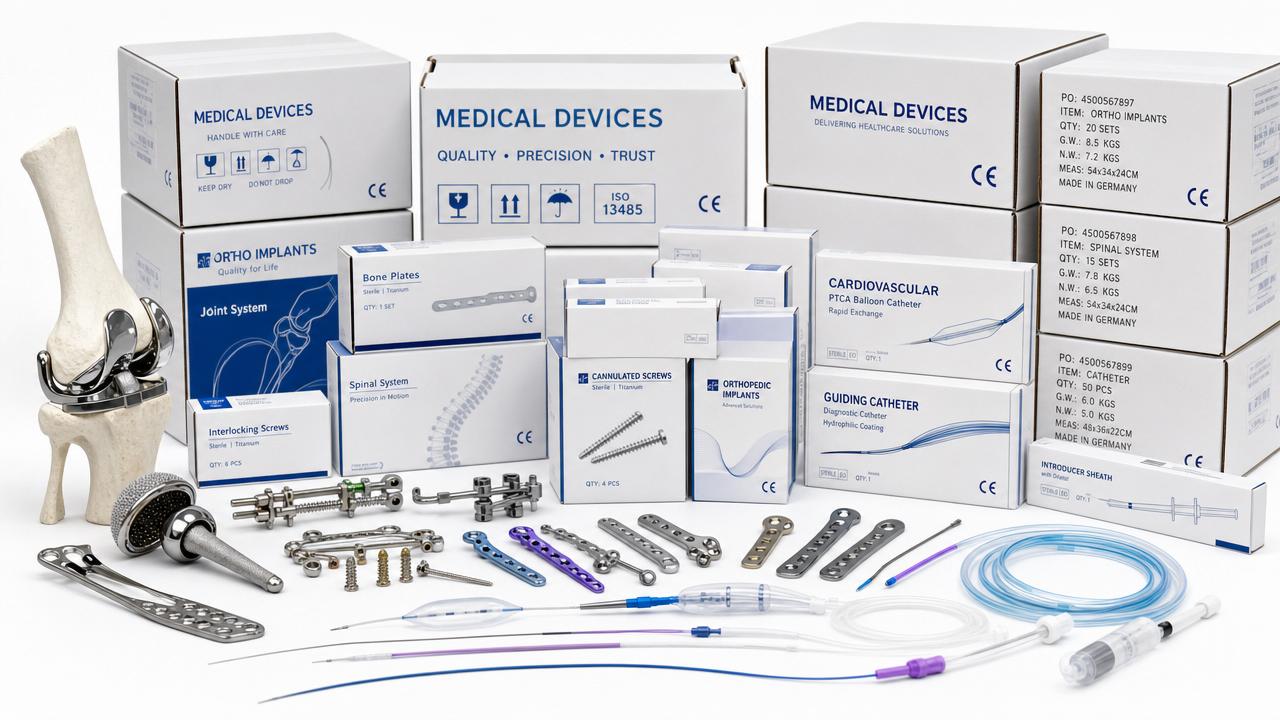
This problem is common across orthopedic implants, cardiovascular interventional devices, stapling systems, polymer catheters, and advanced wound care. Each category has different risk profiles, but the late-gap pattern is remarkably similar.
- Clinical claims were drafted from marketing language instead of evidence boundaries.
- Equivalent device comparisons were assumed to be sufficient, but technical and clinical comparability was weak.
- ISO 10993, usability, sterilization, and shelf-life outputs were generated in silos, leaving the clinical story fragmented.
- Post-market surveillance data existed, but it was not structured to answer benefit-risk questions.
- Submission teams underestimated how regulators assess long-term safety, residual risk, and state of the art.
When these disconnects surface late, the result is not only schedule pressure. It can also affect procurement planning, launch sequencing, and pricing strategy, especially in markets influenced by strict reimbursement control or VBP pressure.
Late findings usually come from cross-functional blind spots
A medical device clinical evaluation is not an isolated clinical writing exercise. It is a structured argument connecting device design, material selection, intended clinical performance, known hazards, literature, complaint trends, and follow-up activities.
That is why IMCS emphasizes intelligence stitching. In Class III and other high-value consumables, micron-level engineering and biocompatibility decisions directly shape what can be defended clinically later.
Where do the biggest medical device clinical evaluation gaps usually appear?
Quality and safety teams can reduce delays by knowing where the most frequent evidence gaps appear. The table below highlights common failure points across high-risk consumable categories and what they mean for submission readiness.
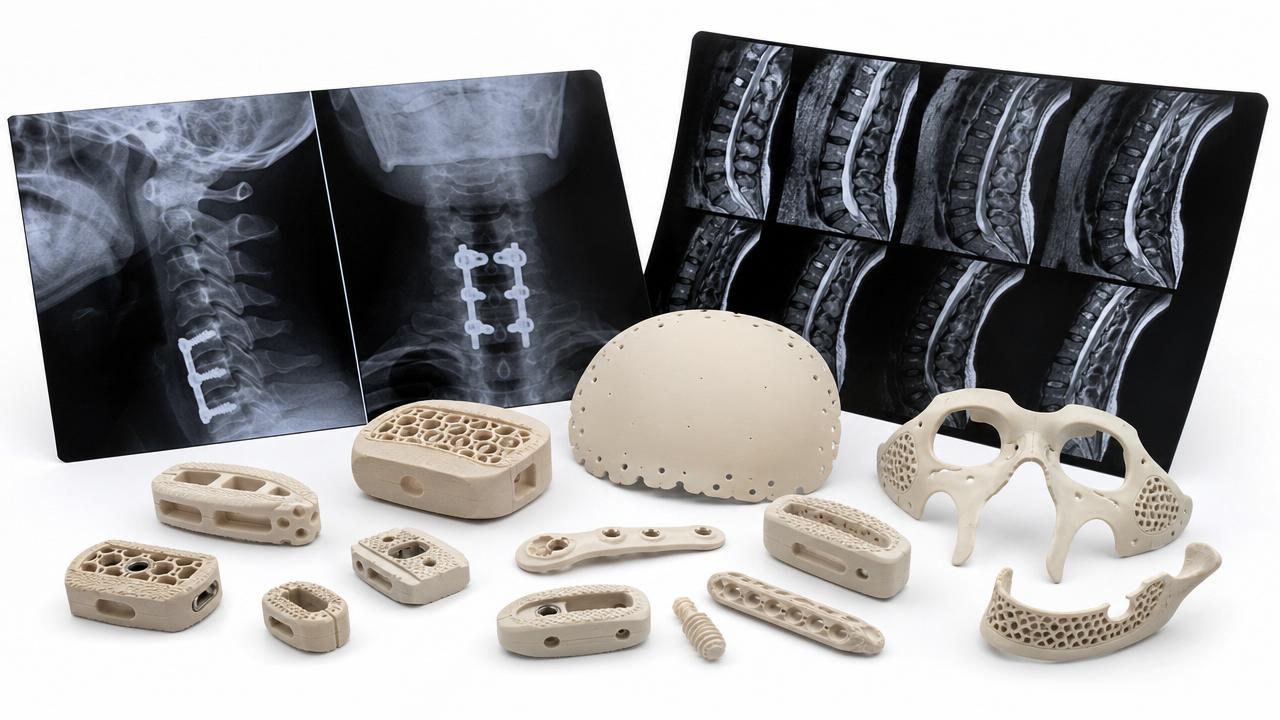
These gaps are not limited to one product family. A porous orthopedic implant may struggle with long-term osseointegration evidence, while a coated catheter may face thrombus, hemocompatibility, or coating durability questions. Different technologies, same clinical evaluation challenge.
Examples by product scenario
- Orthopedic implants: insufficient linkage between surface architecture, wear profile, and clinical survivorship expectations.
- Cardiovascular devices: limited justification for lesion complexity, antiplatelet therapy assumptions, or long-term adverse event profile.
- Staplers: weak support for tissue thickness range, staple line integrity, and complication comparability across procedures.
- Polymer catheters: gaps between bench performance and clinically meaningful endpoints such as dwell time, thrombosis, or vessel trauma.
- Advanced dressings: overextended healing claims without adequate support for wound type, exudate management, or infection-related outcomes.
How should quality and safety managers review medical device clinical evaluation readiness?
A useful review starts before the CER is written. It begins when claims, materials, contact profile, and user environment are still being defined. For quality and safety leaders, readiness means being able to defend consistency, not just completeness.
The following checklist can be used during development transfer, design review, or pre-submission preparation to identify medical device clinical evaluation issues before they become critical.
- Confirm whether the intended use, target population, anatomical site, duration, and contraindications are identical across labeling, risk files, and clinical documents.
- Map every performance claim to supporting evidence, including bench data, animal data if relevant, clinical literature, and post-market signals.
- Check whether biological safety conclusions under ISO 10993 align with the actual clinical contact scenario and manufacturing residues.
- Review equivalence arguments against material chemistry, design geometry, deployment method, and clinical performance endpoints.
- Assess whether complaint handling and vigilance data are coded in a way that supports benefit-risk updates and PMCF planning.
This cross-check is especially important for manufacturers balancing global registrations, multiple sterilization sites, or supplier changes. Small design or process adjustments can undermine an earlier medical device clinical evaluation strategy.
What mature teams do differently
More mature organizations do not wait for notified body questions or internal audit findings. They define a clinical evidence architecture early, then update it whenever materials, coatings, indications, or process controls change.
At IMCS, this is where regulatory and technical intelligence matter most. A device made from advanced polymers or porous titanium structures may look stable from an engineering perspective, but the submission path depends on how those properties are translated into defendable clinical meaning.
Medical device clinical evaluation versus late-stage patching: what is the real cost?
Late-stage patching often appears cheaper because it avoids early investment. In reality, it tends to create more expensive cycles of literature rework, expanded testing, claim reduction, consultant escalation, and lost market timing.
The comparison below helps quality and safety teams explain this trade-off internally, especially when procurement, finance, and regulatory functions are not aligned on evidence planning priorities.
For manufacturers exposed to pricing compression, delayed approval does not only defer revenue. It can weaken tender readiness, disrupt distributor confidence, and narrow the premium positioning that high-value consumables depend on.
Why this matters in VBP and cost-control markets
Where procurement systems reward scale and price discipline, a delayed or narrowed clinical dossier can remove strategic flexibility. Clinical defensibility supports not only approval but also differentiation, hospital adoption, and evidence-based pricing discussions.
Which standards and evidence sources should anchor a stronger clinical evaluation?
A stronger medical device clinical evaluation does not come from literature volume alone. It comes from coherent use of standards, risk files, technical data, and post-market evidence. Teams need a documented logic for why each evidence source is relevant and sufficient.
- Clinical evaluation framework and CER expectations under applicable regional regulations, including CE MDR where relevant.
- ISO 14971 for risk management integration, ensuring hazards and residual risks are clinically interpreted rather than listed mechanically.
- ISO 10993 series for biological safety, especially where materials, coatings, leachables, or long-duration contact create clinical concern.
- Usability, sterilization, packaging, and shelf-life standards that influence real-world performance and adverse event probability.
- Complaint, vigilance, registry, and PMCF sources that show how the device performs outside controlled validation settings.
This is particularly important for sophisticated consumables. A DES, TAVR component, PEEK spinal device, or anti-thrombotic catheter may require a tighter chain of logic between technical properties and patient-relevant outcomes than a lower-risk product.
A practical evidence hierarchy for review teams
When resources are limited, prioritize evidence that directly answers regulatory doubt. Ask which data best explains safety over contact duration, performance in intended anatomy, and residual risk under foreseeable misuse or procedural variation.
How can IMCS help identify clinical evaluation risk earlier?
IMCS works at the intersection of materials science, precision manufacturing, regulatory logic, and market pressure. That combination matters because medical device clinical evaluation gaps are rarely only clinical. They are usually technical, quality, and commercial at the same time.
For orthopedic implants and instruments, early review may focus on material biocompatibility boundaries, porous structure claims, wear relevance, and long-term fixation logic. For cardiovascular devices, it may center on lesion applicability, access profile, thrombogenicity, and adverse event comparability.
For staplers, catheters, and advanced dressings, the review often needs to connect device design and handling characteristics with clinically meaningful endpoints rather than generic performance statements. That is where many internal files look complete yet remain difficult to defend externally.
- Gap screening between intended use, CER logic, risk files, and biological safety conclusions.
- Evidence planning support for Class III implants and high-value consumables before submission bottlenecks emerge.
- Cross-functional interpretation of ISO 10993, CER expectations, and post-market data relevance.
- Strategic input where compliance timing affects procurement windows, pricing pressure, or VBP participation planning.
FAQ: what do quality and safety managers ask most about medical device clinical evaluation?
How early should a medical device clinical evaluation strategy start?
It should start when intended use, material selection, and core claims are first defined. If the strategy begins only at submission drafting, teams may discover that existing verification data cannot support the clinical story they want to make.
Can literature alone support a Class III medical device clinical evaluation?
Sometimes, but only when equivalence and applicability are robustly justified. For many Class III devices, literature may support part of the argument, while additional PMCF, registry data, or device-specific evidence is still needed to close residual uncertainty.
What is the most common hidden gap in a CER package?
A frequent hidden gap is inconsistency. The CER may state one target population, the IFU another, and the risk file a broader hazard profile. Regulators notice these contradictions quickly, and they often trigger deeper review.
How does post-market data improve clinical evaluation quality?
Post-market data helps confirm real-world safety and performance trends, reveal rare complications, and validate whether risk controls remain effective in routine practice. It is especially useful when bench success does not fully explain long-term clinical outcomes.
Why choose us for earlier clinical evaluation planning?
If your team is preparing a Class III dossier, updating a CER, reviewing equivalence, or managing a design change that may affect submission logic, IMCS can help you assess the medical device clinical evaluation path before delays become expensive.
You can consult with us on evidence mapping, claim boundary review, ISO 10993 alignment, product category risk interpretation, submission-readiness checks, and the likely impact of clinical gaps on procurement timing or market access strategy.
We also support discussions around product selection logic, delivery timeline risk, documentation priorities, certification expectations, sample evaluation pathways, and quotation planning for high-value medical consumables. For quality and safety managers, the goal is simple: identify the weak points early, defend the dossier clearly, and protect both compliance and commercial timing.
Get weekly intelligence in your inbox.
No noise. No sponsored content. Pure intelligence.
News Recommendations